Indian American Women Overlooked in Escalating Breast Cancer Crisis
A recent report has issued urgent warnings about Indian American women being "unscreened and overlooked" regarding breast cancer risk. This issue stems from cultural norms, significant data gaps, and evolving disease patterns, posing a severe and under-recognized health crisis in the United States.
Rising Incidence and Unequal Progress in Breast Cancer
Breast cancer remains one of the most prevalent cancers affecting women in the US, accounting for approximately 16% of all new cancer diagnoses and serving as a leading cause of cancer-related deaths among women, according to KFF, a prominent health policy organization. While overall advancements in screening and treatment have substantially reduced mortality rates over recent decades, these benefits have not been distributed equally across all ethnic groups.
For Asian Americans and Pacific Islanders (AAPI), a broad category that includes Indian Americans, recent data from the Breast Cancer Research Foundation indicates that breast cancer incidence is rising more rapidly than in other groups, particularly among women under 50. However, Indian American women are especially poorly tracked in health surveillance systems, as census and health data often aggregate them with other Asian subgroups, obscuring true risk patterns.
Factors Driving Increased Risk Among Indian American Women
Historically, breast cancer was viewed primarily as a disease affecting older women. Yet, national cancer registry data reveal that rates of new breast cancers have surged among younger Asian American women, especially those under 50, with increases exceeding 50% between 2000 and 2021 in some AAPI subgroups.
For Indian American women specifically, this trend is compounded by a mix of biological, lifestyle, and cultural factors. Research suggests that adopting Western diets, sedentary lifestyles, delayed childbirth, shorter breastfeeding durations, and higher overall estrogen exposure can elevate breast cancer risk. These shifts in reproductive and lifestyle patterns are becoming more prevalent among Indian American women as they settle in the US, potentially heightening their long-term vulnerability.
AAPI women, including those of Indian descent, are more likely to have dense breast tissue, which not only increases cancer risk but also makes small tumors harder to detect on mammograms. Cultural norms surrounding healthcare, language barriers, lack of awareness about preventive medicine, and limited confidence in the US health system all contribute to reduced participation in regular screening. For many first-generation Indian American women, it remains common to visit a doctor only when symptoms appear, rather than for preventive care.
Disparities in Screening and Consequences of Late Diagnosis
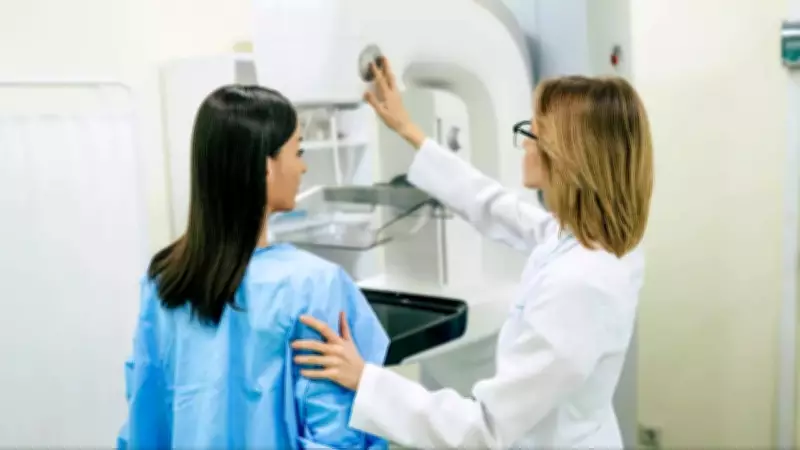
Regular breast cancer screening, primarily through mammograms, significantly enhances early detection, enabling less invasive treatments and much higher survival rates. However, data reveal substantial disparities in screening participation across racial and ethnic groups. Nationwide, about 78.5% of US women aged 50–74 report having a recent mammogram, according to Behavioral Risk Factor Surveillance System (BRFSS) data sponsored by the Centers for Disease Control and Prevention (CDC).
Among specific minority populations like American Indian/Alaska Native women, screening rates can be markedly lower. For AAPI women, including Indian Americans, CDC data indicate some of the lowest mammography rates, with only approximately 54% reporting a mammogram in the past two years, below the national average and trailing other major groups.
These gaps mean cancers are more likely to be diagnosed at later stages among unscreened women, reducing treatment options and survival prospects. Early detection is particularly crucial because breast cancer incidence is rising fastest among younger women, who may not yet be targeted by routine screening recommendations.
Why Indian American Women Are "Overlooked" in Health Data
A core issue is that Indian Americans often do not appear separately in cancer statistics. In health reporting, they are typically counted under the broader Asian American category, masking subgroup differences. This lack of disaggregated data complicates efforts by public health agencies to identify risk patterns specifically affecting South Asian communities and to tailor screening and outreach initiatives accordingly.
Without clear data, Indian American women can be excluded from targeted prevention campaigns, even as their risk escalates. Cultural factors also influence how women perceive and respond to health information. In some Indian American communities, discussions about breast health remain infrequent, and preventive screenings may not be prioritized until symptoms emerge.
Other barriers include:
- Language challenges that hinder understanding of health recommendations.
- Modesty and stigma around discussing breast health, which may delay clinical exams.
- Distrust or unfamiliarity with preventive medical practices common in the US health system.
Addressing these cultural and knowledge barriers through community education, physician outreach, and culturally sensitive messaging is critical to closing the screening gap.
Strategies to Mitigate Breast Cancer Risk Among Indian American Women
Early-stage breast cancer is far more treatable than advanced disease. When mammograms lead to early diagnosis, women often require less aggressive treatment and enjoy significantly higher survival rates. Moreover, breast cancer incidence among younger women is increasing, a trend observed across racial groups and particularly sharp among Asian Americans, reinforcing the need for awareness and regular screening before symptoms appear.
Public health agencies like the CDC and advocacy groups emphasize that mammography and regular clinical breast exams remain the cornerstone of early detection and mortality reduction for breast cancer. Experts recommend several strategies to tackle this overlooked risk:
- Better Data Collection - Segregating health data for Indian American women, instead of lumping them under broader Asian categories, would help identify true incidence, screening rates, and outcomes.
- Community Outreach and Education - Culturally tailored education campaigns can raise awareness about breast cancer risk, the importance of regular screening, and how to navigate the US health system for preventive care.
- Accessible Screening Services - Mobile mammography units, insurance coverage for screening, and local health partnerships can improve access for women who might otherwise delay or skip screenings.
- Normalizing Conversations - Public figures, community leaders, and health influencers in Indian American communities can help destigmatize breast health discussions and encourage proactive care.
Breast cancer rates are rising fastest among Asian American women in the US, especially those under age 50, yet Indian American women remain poorly represented in data and underserved in screening outreach. Screening rates for mammograms are lower among some minority groups, including AAPI women, contributing to later diagnoses and poorer outcomes. Cultural barriers, lifestyle changes, and lack of disaggregated data all contribute to Indian American women being "overlooked" despite increasing risk. Early detection saves lives, and improving targeted screening and awareness could dramatically shift outcomes for Indian American women.