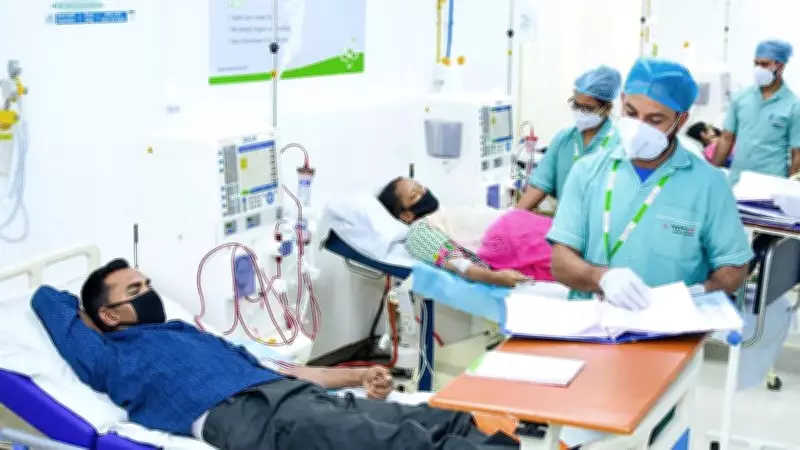
In-Hospital Dialysis for Critical Patients: Prioritizing Safety and Monitoring
In-hospital dialysis for critical patients is a life-sustaining procedure that demands meticulous attention to safety and continuous monitoring. This medical intervention, often required for individuals with acute kidney injury or severe chronic kidney disease, involves complex protocols to ensure patient well-being and prevent complications. As healthcare facilities strive to enhance renal care, understanding the key considerations for in-hospital dialysis becomes paramount for medical teams and administrators alike.
Critical Safety Measures in Dialysis Procedures
The safety of critical patients undergoing dialysis hinges on several foundational elements. Infection control is a top priority, as these patients are often immunocompromised and susceptible to bloodstream infections. Strict adherence to aseptic techniques during catheter insertion and maintenance, along with regular disinfection of dialysis equipment, is essential to minimize infection risks. Additionally, water quality management plays a crucial role, as contaminated dialysate can lead to serious adverse events, including sepsis or inflammatory reactions.
Another vital aspect is hemodynamic stability. Dialysis can cause significant fluid shifts and blood pressure fluctuations, which are particularly dangerous for critically ill patients with compromised cardiovascular systems. To mitigate this, healthcare providers must carefully calculate ultrafiltration rates and monitor vital signs continuously during sessions. The use of advanced monitoring technologies, such as non-invasive cardiac output devices, can aid in real-time assessment and adjustment of treatment parameters.
Comprehensive Monitoring Protocols for Optimal Outcomes
Effective monitoring during in-hospital dialysis involves a multi-faceted approach to track patient responses and intervene promptly when needed. Key components include:
- Vital Sign Surveillance: Continuous monitoring of blood pressure, heart rate, oxygen saturation, and temperature to detect early signs of instability, such as hypotension or hypoxemia.
- Laboratory Parameter Tracking: Regular assessment of electrolyte levels, blood urea nitrogen, and creatinine to evaluate dialysis adequacy and prevent imbalances like hyperkalemia or acidosis.
- Neurological and Pain Assessment: Observing for symptoms of dialysis disequilibrium syndrome, such as headaches or confusion, and managing pain or discomfort to improve patient comfort and compliance.
Moreover, staff training and competency are indispensable for successful monitoring. Dialysis nurses and technicians must be proficient in operating dialysis machines, recognizing alarm signals, and responding to emergencies. Ongoing education on the latest guidelines and simulation-based drills can enhance team preparedness and reduce human error.
Addressing Challenges and Enhancing Patient Care
In-hospital dialysis for critical patients presents unique challenges that require tailored strategies. For instance, patients with multi-organ failure may need integrated care plans that coordinate dialysis with other treatments, such as mechanical ventilation or inotropic support. Communication and documentation are critical in this context; clear handoffs between ICU and dialysis teams, along with detailed electronic health records, ensure continuity of care and reduce the risk of medication errors or missed interventions.
Furthermore, patient and family education contributes to safety by empowering them to report symptoms or concerns. Explaining the dialysis process, potential side effects, and the importance of adherence to treatment schedules can foster collaboration and improve overall outcomes. As healthcare evolves, leveraging data analytics to predict complications and personalize dialysis regimens holds promise for advancing renal care in critical settings.
In conclusion, in-hospital dialysis for critical patients requires a robust framework of safety measures and vigilant monitoring to safeguard against risks and optimize therapeutic benefits. By focusing on infection prevention, hemodynamic management, and comprehensive surveillance, healthcare providers can deliver high-quality dialysis care that supports patient recovery and enhances survival rates in intensive care environments.