Chronic Venous Insufficiency: A Comprehensive Guide to the Circulatory Disorder
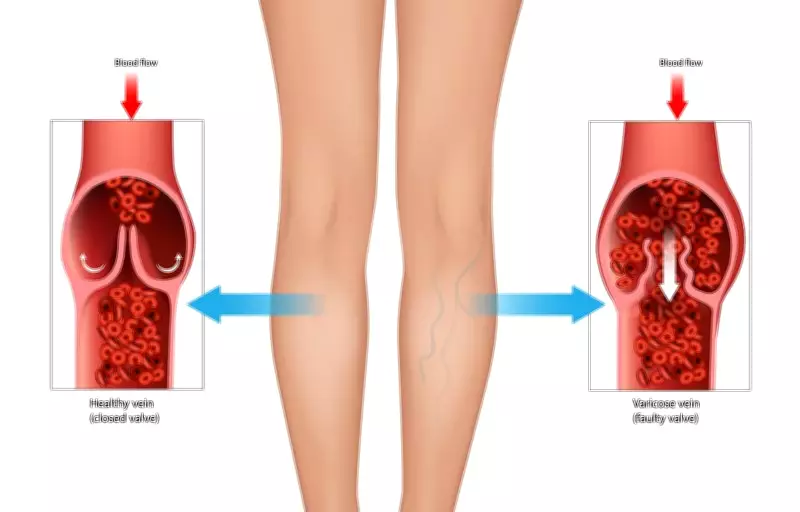
Chronic Venous Insufficiency, commonly abbreviated as CVI, represents a significant medical condition affecting the circulatory system, particularly in the lower extremities. This disorder occurs when the venous valves within the legs become weakened, damaged, or dysfunctional, losing their crucial ability to efficiently direct blood flow upward toward the heart. As a consequence, blood tends to accumulate and pool in the lower legs, resulting in elevated venous pressure and a range of distressing symptoms that can severely impact quality of life.
Understanding the Mechanism of Venous Reflux
The primary issue in Chronic Venous Insufficiency revolves around a phenomenon known as venous reflux or venous incompetence. In healthy individuals, veins in the legs contain one-way valves that prevent blood from flowing backward due to gravity. When these valves fail, blood refluxes downward, leading to venous hypertension. This increased pressure within the veins causes them to stretch and enlarge, often becoming varicose veins, and contributes to fluid leakage into surrounding tissues.
Symptoms and Clinical Manifestations
Patients with CVI typically experience a variety of symptoms that progressively worsen if left untreated. The most common initial signs include persistent leg swelling, especially around the ankles and calves, which may worsen after prolonged standing or sitting. Other frequent symptoms encompass:
- Heavy, aching, or tired sensations in the legs
- Itching or tingling sensations around affected veins
- Skin changes such as discoloration, thickening, or inflammation
- Development of venous ulcers, particularly near the ankles
- Varicose veins that are visibly enlarged and twisted
In advanced stages, Chronic Venous Insufficiency can lead to serious complications like leg ulcers that are difficult to heal, deep vein thrombosis, and significant pain that limits mobility.
Risk Factors and Preventive Measures
Several factors increase the likelihood of developing Chronic Venous Insufficiency. These include advanced age, obesity, pregnancy, a family history of venous diseases, prolonged standing or sitting occupations, and previous leg injuries or surgeries. To mitigate risks, healthcare professionals recommend maintaining a healthy weight, engaging in regular physical activity to promote calf muscle pump function, elevating legs when resting, and wearing compression stockings if prone to venous issues.
Diagnosis and Modern Treatment Approaches
Diagnosis of CVI typically involves a thorough medical history, physical examination, and specialized tests such as duplex ultrasound to assess blood flow and valve function. Treatment strategies vary based on severity but often include conservative measures like compression therapy, lifestyle modifications, and medications to reduce swelling. For more severe cases, minimally invasive procedures like endovenous ablation or sclerotherapy may be employed to close malfunctioning veins, while surgical options remain available for complex situations.
Chronic Venous Insufficiency represents a prevalent yet often underdiagnosed condition that requires timely medical attention. With proper management, most patients can achieve significant symptom relief and prevent progression to more serious complications, highlighting the importance of awareness and early intervention in venous health.